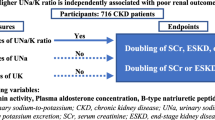
Abstract
Cardiovascular risk profiling and therapy have traditionally been based on established risk factors, such as age, smoking, sex, hypertension, dyslipidemia, body weight, and diabetes mellitus. Despite optimum therapy, cardiovascular mortality and morbidity remain high. Attention is being devoted, therefore, to identifying new risk factors that can also be used as therapeutic targets. Renal dysfunction manifesting as low glomerular filtration rate, albuminuria, or anemia is a strong risk factor for cardiovascular disease and is prevalent in the general population and among patients with cardiovascular disease. Epidemiological data suggest that 10–11% of the general population have low glomerular filtration rates, 5–7% have increased urinary albumin excretion, and 5–10% have anemia. Each of these features represents an independent but additive cardiovascular risk. Treatments for all these indications can reduce cardiovascular mortality and morbidity as well as renal risk. Such findings suggest that treatment should be directed towards improving renal function in order to achieve optimum cardiovascular benefit. Such a strategy would offer the possibility of multiorgan therapy in diseases characterized by multiorgan impairment, such as type 2 diabetes. I present the evidence that renal dysfunction is a common and powerful cardiovascular risk factor and that treatment strategies intervening in the renin–angiotensin–aldosterone system can be used to target albuminuria and reduce cardiovascular and renal risk.
Key Points
-
Increasingly, data show that renal dysfunction is a strong predictor of cardiovascular mortality and morbidity in the general population and among patients with cardiovascular or renal disease, and that cardiovascular disease has an adverse effect on renal function
-
The three main manifestations of renal dysfunction—low glomerular filtration rate, microalbuminuria, and anemia—have independent, additive effects on the risk of renal and cardiovascular disease progression
-
Therapies acting on the renin–angiotensin–aldosterone system have been shown to exert benefits beyond blood pressure reduction in relation to cardiovascular and renal endpoints
-
Patients with renal impairment have frequently been excluded from studies of treatment strategies aimed at the renin–angiotensin–aldosterone system, although growing evidence suggests they are appropriate candidates for these therapies
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Wilson PW et al. (1998) Prediction of coronary heart disease using risk factor categories. Circulation 97: 1837–1847
Conroy RM et al. (2003) Estimation of ten-year risk of fatal cardiovascular disease in Europe: The SCORE project. Eur Heart J 24: 987–1003
Hovens MM et al. (2005) Pharmacological strategies to reduce cardiovascular risk in type 2 diabetes mellitus: an update. Drugs 65: 433–445
De Zeeuw D et al. (2005) The kidney, a cardiovascular risk marker, and a new target for therapy. Kidney Int Suppl: S25–S29
Smith GL et al. (2006) Renal impairment and outcomes in heart failure: Systematic review and meta-analysis. J Am Coll Cardiol 47: 1987–1996
Coresh J et al. (2003) Prevalence of chronic kidney disease and decreased kidney function in the adult US population: Third National Health and Nutrition Examination Survey. Am J Kidney Dis 41: 1–12
Pinto-Sietsma SJ et al. (2000) Urinary albumin excretion is associated with renal functional abnormalities in a nondiabetic population. J Am Soc Nephrol 11: 1882–1888
Tapp RJ et al. (2004) Albuminuria is evident in the early stages of diabetes onset: Results from the Australian Diabetes, Obesity, and Lifestyle Study (AusDiab). Am J Kidney Dis 44: 792–798
Hallan H et al. (2003) Microalbuminuria in diabetic and hypertensive patients and the general population—consequences of various diagnostic criteria—the Nord-Trøndelag Health Study (HUNT). Scand J Urol Nephrol 37: 151–158
National Kidney Foundation (2002) K/DOQI clinical practice guidelines for chronic kidney disease: Evaluation, classification, and stratification. Am J Kidney Dis 39 (Suppl 1): S1–S266
Santoro A (2002) Anemia in renal insufficiency. Rev Clin Exp Hematol Suppl 1: 12–20
Iseki K et al. (2003) Haematocrit and the risk of developing end-stage renal disease. Nephrol Dial Transplant 18: 899–905
Hall WD (1999) A rational approach to the treatment of hypertension in special populations. Am Fam Physician 60: 156–162
Jones CA et al. (1998) Serum creatinine levels in the US population: Third National Health and Nutrition Examination Survey. Am J Kidney Dis 32: 992–999
Yuyun MF et al. (2004) Microalbuminuria, cardiovascular risk factors and cardiovascular morbidity in a British population: The Epic-Norfolk Population-based Study. Eur J Cardiovasc Prev Rehabil 11: 207–213
Atkins RC et al. (2004) Prevalence of albuminuria in Australia: The AusDiab Kidney Study. Kidney Int Suppl: S22–S24
Hillege HL et al. (2004) Cystatin C, a novel marker for mortality in the general population: Data obtained from The PREVEND Study [abstract]. J Am Coll Cardiol 43: 519A
Filler G et al. (2005) Cystatin C as a marker of GFR—history, indications, and future research. Clin Biochem 38: 1–8
Go AS et al. (2004) Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 351: 1296–1305
Levey AS et al. (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130: 461–470
Shulman NB et al. (1989) Prognostic value of serum creatinine and effect of treatment of hypertension on renal function. Results from the hypertension detection and follow-up program. The Hypertension Detection and Follow-up Program Cooperative Group. Hypertension 13 (Suppl): I80–I93
Hillege HL et al. (2003) Accelerated decline and prognostic impact of renal function after myocardial infarction and the benefits of ACE inhibition: The CATS Randomized Trial. Eur Heart J 24: 412–420
Remuzzi G et al. (2004) Continuum of renoprotection with losartan at all stages of type 2 diabetic nephropathy: a post hoc analysis of the RENAAL trial results. J Am Soc Nephrol 15: 3117–3125
Kannel WB et al. (1984) The prognostic significance of proteinuria: The Framingham Study. Am Heart J 108: 1347–1352
Hillege HL et al. (2002) Urinary albumin excretion predicts cardiovascular and noncardiovascular mortality in general population. Circulation 106: 1777–1782
Romundstad S et al. (2003) Microalbuminuria and all-cause mortality in 2,089 apparently healthy individuals: A 4.4-year follow-up study. The Nord-Trøndelag Health Study (HUNT), Norway. Am J Kidney Dis 42: 466–473
Borch-Johnsen K et al. (1999) Urinary albumin excretion. An independent predictor of ischemic heart disease. Arterioscler Thromb Vasc Biol 19: 1992–1997
Arnlov J et al. (2005) Low-grade albuminuria and incidence of cardiovascular disease events in nonhypertensive and nondiabetic individuals: the Framingham Heart Study. Circulation 112: 969–975
Wachtell K et al. (2003) Albuminuria and cardiovascular risk in hypertensive patients with left ventricular hypertrophy: the LIFE Study. Ann Intern Med 139: 901–906
De Zeeuw D et al. (2004) Albuminuria, a therapeutic target for cardiovascular protection in type 2 diabetic patients with nephropathy. Circulation 110: 921–927
Collins AJ (2003) The hemoglobin link to adverse outcomes. Advanced Studies in Medicine 3 (Suppl): S194–S197
Levin A et al. (1999) Left ventricular mass index increase in early renal disease: Impact of decline in hemoglobin. Am J Kidney Dis 34: 125–134
McClellan WM et al. (2002) Anemia and renal insufficiency are independent risk factors for death among patients with congestive heart failure admitted to community hospitals: A population-based study. J Am Soc Nephrol 13: 1928–1936
Dahlöf B et al. (2002) Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 359: 995–1003
Yusuf S et al. (2000) Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N Engl J Med 342: 145–153
Lewis EJ et al. (2001) Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 345: 851–860
Parving HH et al.; Irbesartan in Patients with Type 2 Diabetes and Microalbuminuria Study Group (2001) The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 345: 870–878
The GISEN Group (Gruppo Italiano Di Studi Epidemiologici In Nefrologia) (1997) Randomised placebo-controlled trial of effect of ramipril on decline in glomerular filtration rate and risk of terminal renal failure in proteinuric, non-diabetic nephropathy. Lancet 349: 1857–1863
Brenner BM et al. (2001) Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 345: 861–869
Mann JF et al. (2001) Renal insufficiency as a predictor of cardiovascular outcomes and the impact of ramipril: The HOPE randomized trial. Ann Intern Med 134: 629–636
Asselbergs FW et al. (2004) Effects of fosinopril and pravastatin on cardiovascular events in subjects with microalbuminuria. Circulation 110: 2809–2816
Ibsen H et al. (2005) Reduction in albuminuria translates to reduction in cardiovascular events in hypertensive patients: losartan Intervention For Endpoint reduction in hypertension study. Hypertension 45: 198–202
Silverberg DS et al. (2003) The effect of correction of anaemia in diabetics and non-diabetics with severe resistant congestive heart failure and chronic renal failure by subcutaneous erythropoietin and intravenous iron. Nephrol Dial Transplant 18: 141–146
Besarab A et al. (1998) The effects of normal as compared with low hematocrit values in patients with cardiac disease who are receiving hemodialysis and epoietin. N Engl J Med 339: 584–590
Singh AK et al. (2006) Correction of anemia with epoetin alfa in chronic kidney disease. N Engl J Med 355: 2085–2098
Drüeke TB et al. (2006) Normalization of hemoglobin levels in patients with chronic kidney disease and anemia. N Engl J Med 355: 2071–2084
Mix TC et al. (2005) Rationale—Trial to Reduce cardiovascular events with Aranesp™ Therapy (TREAT): Evolving the management of cardiovascular risk in patients with chronic kidney disease. Am Heart J 149: 408–413
Acknowledgements
PAREXEL MMS provided writing assistance, comprising preparation of a draft from slides and audio transcript, preparation of figures and obtaining copyright permissions, proofreading, and reference checking.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
de Zeeuw, D. Renal disease: a common and a silent killer. Nat Rev Cardiol 5 (Suppl 1), S27–S35 (2008). https://doi.org/10.1038/ncpcardio0853
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpcardio0853